Hacettepe University Faculty of Medicine
Department of Chest Diseases
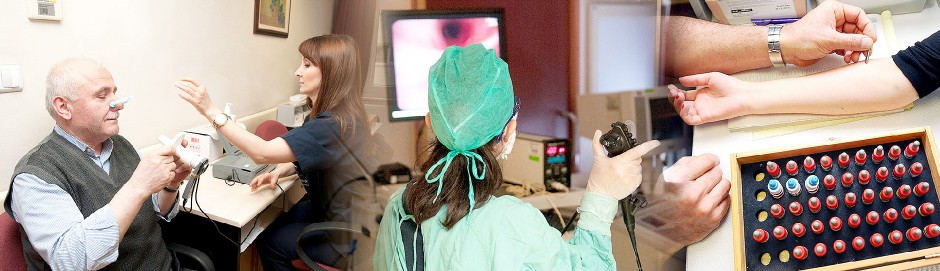
Department of Chest Diseases was founded by esteemed teacher Prof. İzzettin Barış in 1969 within the Department of Internal Medicine. It was separated from Internal Medicine to become an independent department in 1990. Allergic Diseases and Immunology Subdivision is affiliated to our Department. Furthermore, our department has been carrying out common training protocols of “Intensive Care” and “Occupational Health and Diseases” subdivisions.
Our department is located in Adult Hospital of Hacettepe University. Outpatient clinic services for diagnosis, treatment and follow-up of all lung diseases are provided in our department. There are no wards or intensive care units that belong to our department. However, patients in need of inpatient or intensive care are hospitalized in Outpatient Clinics of Internal Medicine or intensive care unit for a multidisciplinary treatment.
Primary diseases which are involved in the diagnosis and treatment field of Chest Diseases Department: asthma, allergic diseases, acute/chronic bronchitis, chronic obstructive pulmonary disease (COPD), lung cancer, pleural diseases, mesothelioma, pulmonary infectious diseases, pneumonia, tuberculosis, interstitial lung disease, sarcoidosis, pulmonary embolism, occupational lung diseases, sleep-disordered breathing and smoking addiction. The treatment plan of patients diagnosed with lung cancer is made upon evaluation in the multidisciplinary thoracic oncology council. All diagnostic and therapeutic procedures in our department are performed by academic staff and residents of Department of Chest Diseases as well as specialist technicians.
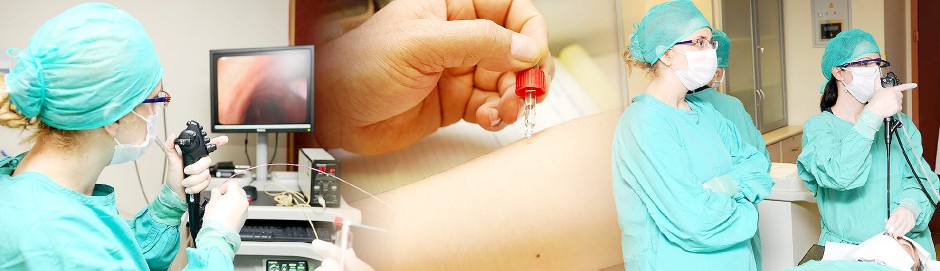
A pulmonary function test laboratory, bronchoscopy units, a laboratory for sleep medicine, thoracic ultrasound, medical thoracoscopy, smoking cessation unit, adult cystic fibrosis unit and Subdivision of Adult Allergic Diseases and Immunology are available in our department.
A spirometer and carbonmonocise diffusion capacity measuring device is available in respiratory function test laboratory. These devices enable respiratory function tests, bronchodilation test and diffusion capacity measurement.
-
• 2 bronchoscopy units are available in our department: one in Adult Hospital and the other in Oncology Hospital Flexible fiberoptic video-bronchoscope and rigid bronchoscope are available in bronchoscopy unit. Bronchoscopy procedure allows displaying the airways, collecting diagnostic biopsies and performing therapeutic interventions. Bronchoscopy offers early and definitive diagnosis of certain pulmonary diseases, particularly lung cancer.
-
• A polysomnography is available in sleep medicine laboratory with a capacity of 2 beds. Polysomnography test is performed for diagnosis and treatment of sleep-disordered breathing. The alterations in breathing during sleep are recorded in a computer-aided media throughout one night.
-
• Medical thoracoscopy enables performing diagnostic and therapeutic interventions for pleural diseases.
-
• A thoracic ultrasound is available in the bronchoscopy unit. Thoracic ultrasound is utilized as an imaging method during thoracentesis procedure and percutaneous lung biopsy.
-
• Furthermore, we perform percutaneous lung biopsy and other invasive procedures in coordination with Interventional Radiology Unit.
-
• The treatment and follow-up of patients who apply for smoking addiction treatment are performed in the outpatient clinic of smoking cessation.
-
• Patients above the age of 18 who are diagnosed with cystic fibrosis are evaluated and followed up in Adult Cystic Fibrosis Unit.
-
• Certain diseases such as allergic rhinitis and asthma, food and drug allergies, insect allergies, atopic dermatitis (eczema), urticaria and angioedema are diagnosed, treated and followed up in Department of Allergic Diseases and Immunology. Skin prick tests and drug allergy tests are performed.
Outpatient clinic services for diagnosis, treatment and follow-up of all lung diseases are provided in our department. Primary diseases which are involved in the diagnosis and treatment field of Chest Diseases Department: asthma, allergic diseases, acute/chronic bronchitis, chronic obstructive pulmonary disease (COPD), lung cancer, pleural diseases, mesothelioma, pulmonary infectious diseases, pneumonia, tuberculosis, interstitial lung disease, sarcoidosis, pulmonary embolism, occupational lung diseases, sleep-disordered breathing and smoking addiction.
The treatment and follow-up of patients who apply for smoking addiction treatment are performed in this private outpatient clinic. Initially we examine our patients and perform lung graphy, respiratory function tests and cardiogram (ECG) as well as blood tests when necessary. Then, we determine the addiction level of the patient and provide psychological support in addition to medical support such as nicotine gums or patches or medication to reduce down the desire to smoke based on the result. We continuously follow up the patients throughout the treatment process and following period of 1 year.
Patients above the age of 18 who are diagnosed with cystic fibrosis are evaluated and followed up. Examinations are given between 13:30-16:00 on Tuesdays and Thursdays in Adult Cystic Fibrosis Unit. Respiratory function tests and microbiological phlegm evaluations are performed quarterly for patients. The frequencies of controls are increased during exacerbation periods. Diabetes and osteoporosis scans, liver-kidney function tests and abdominal ultrasonography, complete blood count as well as measuring levels of immunoglobulin and vitamin in blood and tuberculosis culture in sputum are performed annually. Patients are treated based on sputum culture reproduction. Patients are referred to the relevant departments for respiratory physiotherapy and diet planning as well as gastroenterological and endocrinologic problems. Multidisciplinary meetings participated by Adult Chest Diseases, Pediatric Chest Diseases and Infectious Diseases are organized on a monthly basis to discuss selected cases.
The test involves measuring lung function with a special device called spirometer. The test is performed during office hours without an appointment. The result is given at the end of the test.
The respiratory function test is performed again in order to evaluate the response to the medication called bronchodilator, which is administered to increase airflow to lungs. The test is performed during office hours without an appointment. The result is given at the end of the test.
Bronchoscopy involves evaluating the major airways in the lungs with a camera that can bend in the end (fiberoptic bronchoscope). The procedure allows directly viewing the airways. The patient should have been evaluated in our department prior to bronchoscopy. Certain additional diagnostic examinations can be performed together with bronchoscopy. Bronchial lavage/bronchoalveolar lavage involves squirting liquid (physiological saline solution) into a specific region of the lung and then collected back for examination during bronchoscopy procedure. Transbronchial forceps lung biopsy involves collecting samples from lung tissue or airways with special biopsy instruments during bronchoscopy procedure. Transbronchial lymph node aspiration involves collecting biopsy from the lymph nodes surrounding the airway with a special needle during bronchoscopy procedure. Your physician decides the sequence of these procedures before or while performing.
Considerations before bronchoscopy procedure: You should keep an empty stomach as of midnight the night before the procedure. However, medication used regularly due to high blood pressure, heart disease or any other diseases can be taken with a little amount of water. Patients with high blood pressure, heart disease or neurologic disease should be evaluated by the attended department before the procedure. Blood test might be required for certain patients before the procedure. The procedure is performed under local anesthesia. The procedure lasts for 15-30 minutes based on the sampling. The patient can leave the hospital after being observed for about 1 hour after the procedure and can eat after 2 hours. The procedure report is given right after the procedure.
Rigid bronchoscopy involves evaluating airways directly with a special rigid bronchoscope. It is performed with local or general anesthesia. It is usually used for removing foreign objects aspirated into airways and local treatment of tumors that obstruct airways.
Considerations before rigid bronchoscopy procedure: It is usually performed with general anesthesia. Therefore, hospitalization is required. You should keep an empty stomach as of midnight the night before the procedure. However, medication used regularly due to high blood pressure, heart disease or any other diseases can be taken with a little amount of water. Patients with high blood pressure, heart disease or neurologic disease should be evaluated by the attended department before the procedure. Blood test might be required for certain patients before the procedure. It lasts for 15–30 minutes based on the procedure to be followed. The patient can leave the hospital after being observed for about 1 hour after the procedure and can eat after 2 hours. The procedure report is given right after the procedure.
Fluid accumulation can occur between the lung membranes called pleura due to certain diseases (pleural effusion). Torasynthesis procedure involves evaluating the fluid with ultrasound after collecting a sample for examination under local anesthesia (diagnostic torasynthesis). In certain cases, a part of this fluid is drained (pleural drainage).
It involves collecting biopsy from the lung membrane that surrounds the interior of ribcage (parietal pleura) with a special needle.
Considerations before pleural biopsy: Appointments for the procedure are booked after an evaluation in our department. Blood test might be required for certain patients before the procedure. The patient should preferably have a full stomach during the procedure. The procedure is performed under local anesthesia. Patient can leave the hospital after a short period of observation.
Percutaneous lung biopsy is collected from peripheral tumoral masses under ultrasonography as fine needle aspiration biopsy under local anesthesia.
It involves imaging the lung surface and the interior of ribcage with special camera introduced into the thoracic cavity with a small incision to the chest wall under local anesthesia, and collecting biopsy. Patient should be hospitalized for a short period of time for the procedure.
The procedure involves obliterating the pleural space with various agents (talc, tetracycline). The patient should be evaluated in the department before the procedure.
This sleep respiratory study is conducted for the diagnosis and treatment plan of respiratory disorders in sleep. Patient should be evaluated and have an appointment in the department for the test. Respiratory changes during sleep are evaluated with computer, and the patient is administered pressure air through nasal airway with a mask for treatment, if necessary (in a way to prevent airway). Technician on call at night will place electrodes on you in order to monitor your sleep, respiration and heart rate, and he/she will wait until the test is completed (08:00 a.m.) in order to ensure an intervention when necessary.
Considerations before sleep test: You are recommended to avoid daytime naps, tea or coffee for a comfortable sleep. Male patients should shave off their beard. You should consult with the physician in charge for any sleep medication you are on. You should not have an all-day visitor for the accuracy of test. You should not bring in metal accessories or electronic devices as these can disrupt the record. You should turn off your mobile telephone and remove your dentures, if any. Patients are given lockers to keep their clothes and belongings. A light meal is recommended before leaving home. Patient should arrive at hospital before 22:00 at the evening of the test. You can receive the summary of information on sleep test (polysomnography test) and hospital admission procedures from the department secretariat. Test result is given by the department within 1 week. Multidisciplinary Sleep Council participated by Otorhinolaryngology Department and Orthodontics Department is held at 11:00 on Mondays. Patients are evaluated at the council for treatment recommendations.
Inner part of the arm is pierced with a fine needle called lancet and liquid test solution is penetrated into the skin. 2 control tests consisting of one positive and one negative test are applied in order to determine the skin reactivity characteristics of the patient. Skin reactivity is measured with a ruler 15 minutes later. A small red circle indicates positive result. This finding is evaluated with the clinical data of patient. Patient should not use any allergy medication (antihistamines) for 20 days before the allergy test.
This test is applied after patients with a possible diagnosis of drug allergy are evaluated in the department. Appointment is required. Patient should arrive at 09:00 a.m. for the scheduled day of test. Initial blood pressure, pulse rate, respiratory rate and peak expiratory flow (PEF) values are measured. The test is initiated with lactose (sugar), the dose of which is gradually increased with intervals of 20 minutes before the test medication is administered. All of the measurements are repeated while PEF is measured in the 5th and 20th minutes. In the event that patient reacts to any dosage (itching /skin rash, swollen skin around eyes and/or lips, difficulty in breathing, hoarseness, swallowing disorder, low blood pressure, increased respiratory rate and decreased PEF value), the test is ended and medical intervention is made when necessary. Patient should bring white cheese and bread as lunch. Any other food is not allowed during test. Test ends at 16:00. Drug allergy card is given to patients who are deemed necessary.
In our department, appointments for examination in outpatient clinic can be scheduled by dialing 444 4 444 and clicking “Online Appointment” link.
Appointments can be scheduled after 14:00 on Wednesdays due to trainings held. Full-day examination is available on the remaining days.
Smoking Cessation Unit
You can dial 444 4 444 , click on “Online Appointment” link or dial 171, which is the smoking cessation line of Ministry of Health.
Department of Chest Diseases is in Ward 71 located on the 1st floor upon entering from door no. 7 in Hacettepe University Adult Hospital. The rooms of academic staff, outpatient clinics of chest diseases, respiratory function laboratory and bronchoscopy unit are available in the department.
Allergic Diseases and Immunology Subdivision is located in the hallway on the right side upon entering from door no. 7 in Hacettepe University Adult Hospital. There are 2 separate secretariats which offer service in Chest Diseases Department and Adult Allergy Unit.
Oncology Hospital Bronchoscopy Unit is in Ward 90 located on -1st floor.
Chest Diseases Department:
Telephone:
+90 (312) 305 15 31 or +90 (312) 305 41 16
Fax: +90 (312) 310 08 09
Oncology Hospital Bronchoscopy Unit
Telephone:
+90 (312) 305 32 31
Allergic Diseases and Immunology Department:
Telephone
+90 (312) 305 17 21







